We were cramped but excited in the corner of the ultrasound room, eager to meet our fifth child for the very first time. These moments during a pregnancy are always swelling with emotion: the thrill of new life tempered by “will everything be ok?”
The procedure was rushed and chaotic. The technician told us there was a “potential complication.” She couldn’t locate the anterior tibial artery. We would need to schedule a “Level 2” ultrasound at a different clinic.
A few days later we arrived for the scheduled visit. Upon checking in, we were assigned to a genetic counselor. But we didn’t know why. We found out that it was due to our third child, Hattie, being diagnosed with craniosynostosis. We were surprised because our own doctor never raised this as a concern. “We don’t need a genetic counselor,” I said. “We’re here for my wife.” But despite my protest we were told we would not be seen without a genetic screening.
Soon we were sitting across the table from a young woman. On the table was an assortment of paper, rulers and stencils. She asked us intrusive questions about our family history: “How many siblings are on Becca’s side? Do they have abnormalities?” As we answered she drew lines, circles, and squares on her paper, denoting relatives and their genders. “How many on Rory’s side?” she asked as she sketched another line. “I have two brothers,” I answered. “Any abnormalities?” “No.” Square. Square. She never looked away from the paper. For a deeply personal discussion, it all felt so impersonal.
“How many children do you have?” Line. “Well, we have an 8-year old boy…”
“Is he healthy?”
“Yes.” Square.
“And a 6-year old girl, healthy.” Circle.
“And a 3-year old girl. She has craniosynostosis.” Triangle.
The woman looked up to reassure us: “That is usually not hereditary. There’s probably nothing to worry about with this pregnancy.” Line. “Do you have any other children?”
“Yes,” Becca started, but I interrupted.
“That triangle,” I said, putting my finger on the drawing. “Her name is Hattie. Her middle name is Joy. We should be so lucky to have another Hattie.”
Meeting Hattie
It was 7:22 AM, one hour after her birth when the decision was made to emergency transfer Harriet Joy Groves to a neonatal intensive care unit in Minneapolis. She was born unable to breath on her own, but we didn’t know that right away. Seconds after being born, nurses whisked her away from her mother’s arms. A brief whimper was all we heard at birth, but no more crying. While Becca was being tended by one doctor, another doctor began checking Hattie’s vitals, suctioning fluids, and listening to her lungs. The doctor could hear fluid, possibly meconium ingested during a difficult 54-hour labor. Her hands and feet were turning blue. Sensors on her foot registered in the low 30’s. I asked what that number was. Blood-oxygen level. I asked what is it supposed to be. Above 90. She was hooked up to oxygen and the nurses turned the dial to 30%. Then 40%. Then 100%.
There are many moments of brief panic during pregnancy, labor and delivery. Becca and I both thought this was procedural, that within a few minutes Hattie would be breathing normally and back in her mother’s arms. But as I watched fear grip the nurses, I felt the pit in my stomach grow. God, where are you?
Minutes away from birth she had a CPAP mask covering her mouth and nose, IV needles in her scalp, and a lead plate under her body as the lab techs set up a chest x-ray.
I remember reaching out holding her tiny hand in that moment and introducing myself: “Harriet. This is your daddy. I love you. I don’t know what else to do right now, so I’m just going to hold your hand.”
* * *
Throughout this pregnancy we made plans for a natural child birth. Being our third, we knew enough that nothing goes according to plan when it comes to babies. But still, we did our best to prayerfully follow God’s leading. And we felt peace about it.
The first detour was Hattie being born 10 days late. In those last weeks Becca would talk about how she started writing the birth story in her head, a great blog post in the making: “So there I was in Econofoods buying the ingredients for peanut butter pie when my water broke…” But each time she would sense God respond: Let Me write this story.
So it was with great anticipation that we waited for this story to play out. But many hours after her water broke, having only irregular contractions, we were forced to induce. This was a difficult, doubting hour, dashing months of hopeful expectations. How is this a better story, God?
Each stage, though, kept getting worse. The late pregnancy and contractions were followed by a malpositioned baby causing excruciating, Pitocin-induced, back labor for 6 hours while Becca tried various positions to turn the baby without success. Finally we ordered the epidural but still the baby did not come for 11 more hours. After losing count of the number of times Becca lost the contents of her stomach, it was finally time to push. The delivering doctor was called in and asked me how long Becca pushed with our last child. “Not long at all. Two pushes.” Everyone was in agreement. Third child, long labor, this was going to be over soon. Which was good because Becca was utterly exhausted. I don’t think I’ve ever seen her more depleted, physically and emotionally. An hour later, the nurses stopped counting off the contractions and the doctor couldn’t stop yawning. Progress had been made, but barely (though we didn’t let Becca know). It had been made clear to us that a c-section was a possibility because of the baby’s position. Now that seemed almost inevitable.
But in the final 15 minutes Becca found her strength and rallied. And to everyone’s surprise the baby was born in the ideal, head-down position.
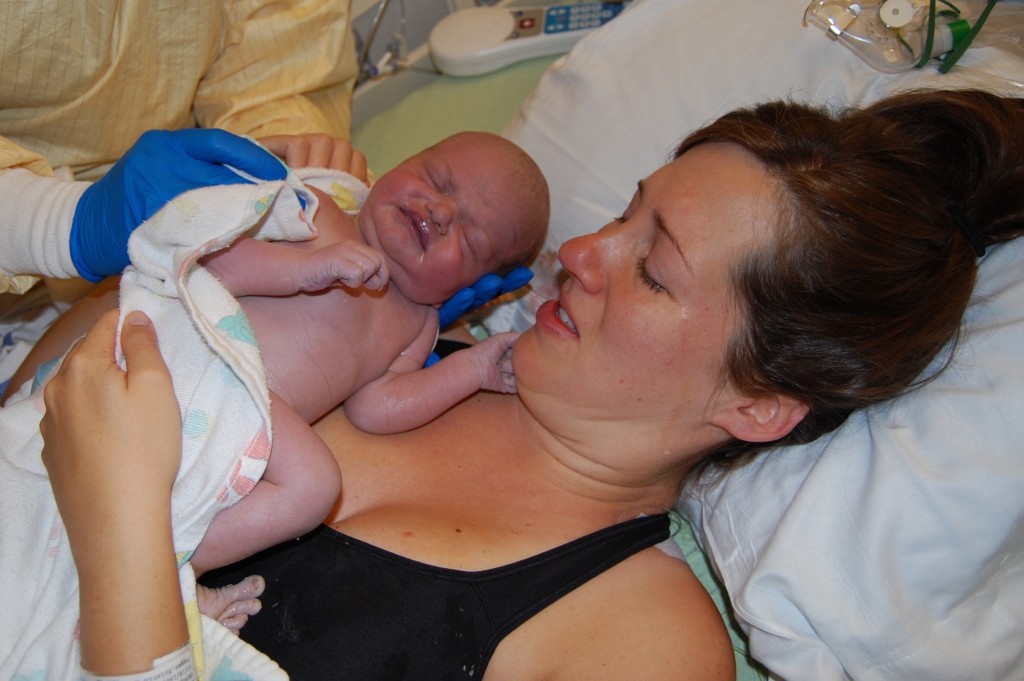
“Cut the cord daddy!” At long last, Harriet had arrived.
* * *
One-half hour after birth the doctors tried to wean Hattie off her supplemental oxygen. Her color was much better but they were unable to keep her stable with less than 40% oxygen. The x-ray had come back showing possible pneumonia in one lung. It was when Hattie started shallow breathing, unable to even keep up with forced oxygen that the head doctor made the emergency call to transfer Hattie to a NICU.
Through tears Becca asked me to call Ali, her close friend from town to come be with her so I could follow Hattie to the other hospital. I stepped into the hallway and called Ali. Then I called our parents. We hadn’t announced Hattie’s birth yet to anyone. If I concentrated I could force the words out, but if I thought about it I was too choked up to talk. “Born 6:22, girl. Trouble breathing. Transferring to NICU in Minneapolis. Please pray.” I remember asking Becca’s mom to pray with our kids who were staying with her. I remember thinking how pure and powerful the prayers of children are, how God hears and is moved by them.
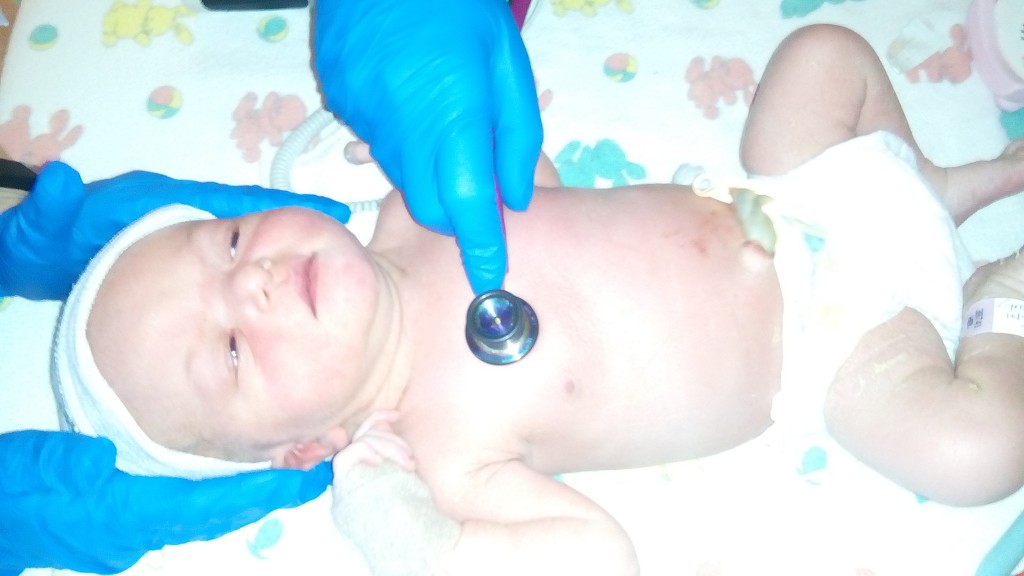
I called my pastor who spread the word to staff and church. All we had left to us now was prayer. We felt so helpless. Becca later told me her frustrated prayers while pushing, You said You began a good work in me. You have to complete it. You said when I am weak, You are strong. I have nothing left. You have to do this.
I returned to the room to pack and get ready to leave with Hattie. She was still rapid-breathing, the doctor listening to her lungs. The nurse explained that the transfer team would bring their own equipment and need to remove the IV’s and monitoring equipment before replacing with their own. As the nurse was preparing Hattie for the transfer she briefly removed the CPAP mask.
As she went to reaffix the mask the doctor stopped her. “Wait.” We all watched the oximeter. It stayed above 90%. The doctor listened to her lungs. “Let’s bring her to Becca.” The nurses looked concerned but promptly complied.

They placed Hattie in Becca’s arms. All our eyes were locked on to the oximeter. Could this be happening? It started rising. 94… 95… 96…
“Let’s try to feed her.” The nurses positioned baby and Becca and she immediately latched on and started nursing. Then she switched sides and kept nursing.
Ali arrived during this scene. I don’t know what I said to her because there wasn’t any explanation. Only minutes had passed since Hattie was rapidly deteriorating. The doctor explained that Hattie might be able to keep this up for 15 minutes, but then she would tire and need to go back on oxygen. We all kept watching the monitors and heard a helicopter in the distance getting louder.
* * *
The transfer team arrived in the room and waited for Hattie to finish nursing before taking their turn to check vitals. I remember thinking how serious these doctors and nurses looked. As grateful as we were to have their help, their arrival made the situation feel all the more overwhelming.
They connected their equipment to Hattie and watched. And we watched them. The doctor listened to Hattie’s chest. “Lungs are clear,” she said. She looked over her a bit longer, then looked at us: “Her stats are perfect.” One of the nurses smiled at me and whispered, “she’s not going to transfer.” After a brief consultation with the hospital doctors, they carried Hattie back to Becca’s arms, packed up their things, and left.
Then God spoke. This is My story.
Within the span of 10 minutes we went from needing an emergency transfer by helicopter to save Hattie’s life to it becoming a precautionary measure to her not needing to be transferred at all. The recovery was instantaneous. She did not get worse and worse and then gradually better, she got worse and worse and worse, then was suddenly healed. Within an hour we were in the postpartum room celebrating with family.

The acting pediatrician later said he’d never heard of a NICU transfer team leaving without the baby before.
When Becca and I (and Hattie) were alone again, all we could do is weep. We knew what we had seen. We knew God had been writing this story all along. We knew that it couldn’t be explained away. We would have never imagined this would be her story. No eye has seen, no ear has heard, no mind has conceived what God has prepared for those who love him.
The Shelter of the Most High
In the years that followed, we made numerous trips to children’s hospitals, geneticists, and other specialists to monitor Hattie’s craniosynostosis (unrelated to her breathing complications at birth). We are very grateful for modern medicine and the dedication of our doctors, but it can be wearisome to face a world that is always trying to “fix” that which is different. Anyone who has spent time in these hospitals knows what I mean. I’ve never seen such fiercely loving parents as I have in children’s hospital waiting rooms.
What was at first a condition requiring invasive neurosurgery became a recommendation to wait-and-see. These visits we were riddled with doubt and fear, but we tried to focus on God’s promises. We memorized Psalm 91 as a family, with a slight alteration, and repeated it often:
I will be with her in trouble,
I will deliver her and honor her,
With long life I will satisfy her
and show her My salvation.
After years of weekly, then monthly, then annual visits to monitor Hattie’s progress, we were told at our last appointment that we do not need to return. “You can keep coming back, and I can keep rubbing Hattie’s head,” the craniofacial doctor told us with a grin, “But you don’t need to.”
That was one year ago, a few months after our fifth child Elias was born. Hattie turned five in October. She is a happy, healthy, joy-filled girl, as everyone who knows her would attest. We are grateful for every precious moment God has given us. We love you, Hattie Joy!

This article appears in the Fall 2020 issue of The Grovestead Newsletter. Please sign up here to receive a complimentary issue.



























4 comments
To GOD be all the glory!!!!!!
May the good LORD take a special likin to Hattie Joy!!!!! (Roy Rodgers)
Blessings and hugs, Jennifern Teshera
Thank you Rory and Becca for sharing this beautiful story of little Hattie. I have some wonderful pictures of Uncle Ben and Hattie, when we visited
a few years ago. Hattie was Ben’s mother’s name and he took a special interest in your little Hattie. I will be glad to send them to you if you want. God is so good. Your blogs and publications are so inspiring. May God continue to guide and direct your lives as you keep trusting and following His leading. I love you all so much. Aunt Jeanette
Thank you so much for sharing Hattie’s story. Through tears and praise I read it. God is good! His mercies endure forever. Your testimony has strengthened my faith! Thank you again!
Wow! What a wonderful story of God’s Faithfulness! Thank you for sharing.